

“People assume that if you wear a facemask you have a disease or communicable virus.” - AHP Panellist
“Because I was wearing a face mask a person thought I was infected and made comments that I should not be out! The public need to be provided with more information about how GOOD facemasks are in reducing transmission.” - AHP Panellist
For August 2020, as the COVID-19 global pandemic continued and the conversation turned towards the use of facemasks to counter the virus, we asked Australia’s Health Panel (AHP) about their attitudes towards facemasks and experiences wearing them in Australia.
We had 157 panellists participate in this survey, with 50 coming from Victoria where the COVID-19 pandemic has had the most significant impact in Australia so far. As with previous AHP surveys the respondents skewed female (75%), aged 46 or older (90%) and living in a major city (61%). Most (68%) self-identified as being in excellent or good health. 48% identified as a Person with a Disability, 19% as Culturally or Linguistically Diverse (CALD), 17% as LGBTIQA+ and 2% as Aboriginal or Torres Strait Islander (ATSI).
figure_1.png
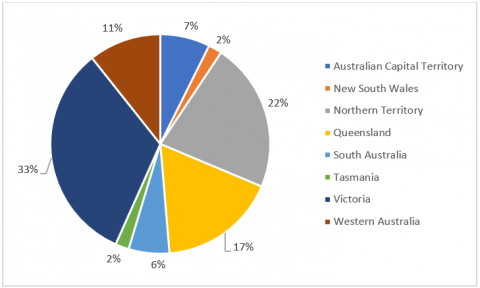
Facemask Efficacy
The substantive majority of panellists (90%) thought facemasks could help limit the spread of COVID-19, while a further 9% thought they maybe could help limit the spread. When asked what kinds of facemasks specifically help, most correctly identified P2/N95 masks (79%), reusable multi-layer cloths masks (73%) and single use surgical masks (70%) as being effective at limiting the spread of COVID-19. 36% reported that any sort of face covering (e.g. scarf, bandana) could be effective and 18% thought single layer cloth mask were effective. This suggests that the messaging around the general efficacy of masks in countering COVID-19 and which specific masks are best has been generally successful.
figure_2.png
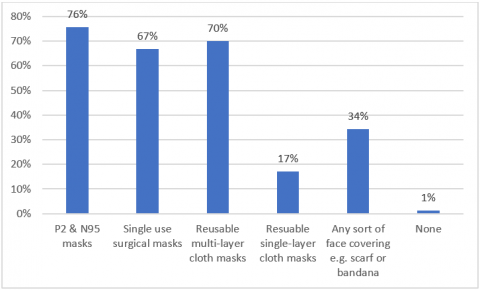
Facemask Usage
When asked how often they wear facemasks when outside of their home, 32% of panellists reported they ‘always’ wear facemasks outside their home, a combined 33% ‘often’ or ‘sometimes’ wear them and the remaining 34% ‘rarely’ or ‘never’ wore a facemask. 33% of panellists reported that they lived/worked in areas where masks are mandatory while only 10% of panellists reported they personally had a medical condition which made it difficult to wear a mask.
figure_3.png
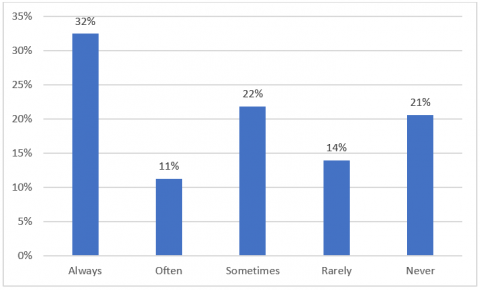
While this initially seems to suggest a fairly even spread of mask usage, the facemask wearing rates vary significantly by location significantly upon further examination. The vast majority of panellists who always wear facemasks (94%) or live/work in areas where facemasks are mandatory (96%) were from Victoria. Conversely, 100% of the panellists who didn’t work/live in an area where facemasks were mandatory or ‘never’, ‘rarely’ or ‘sometimes’ wore a facemask when outside their own home were from outside Victoria.
Focusing on the Victorian respondents (n=50), 90% always wore a facemask outside their home while 10% often wore a mask outside their home. 0% reported ‘sometimes’, ‘rarely’ or ‘never’ wearing a mask.
Concurrently of the panellists from NSW (n=33), another jurisdiction that has been significantly impacted by COVID, usage of masks was still mixed but higher than the national average: 39% always/often wore a mask, 42% sometimes wore a mask, 15% rarely wore a mask and 0% never wore a mask.
This indicates that facemask usage is, perhaps unsurprisingly, strongly related to the perceived personal risk of contracting COVID-19 and Government requirements or recommendation to wear them. It also suggests there are minimal efforts taken by people to wear facemasks as a precautionary measure in places where there are not known outbreaks or explicit requirements, making it critical that Governments effectively track and communicate locations where COVID-19 has been detected.
Facemask Experience
Only 9% of people reported a negative reaction from a member of the public for wearing a facemask, while no panellists (0%) reported being turned away from a business or service for wearing a facemask. Conversely only 6% of panellists reported a negative reaction for NOT wearing a facemask and 3% reported they had been turned away from a business or service for NOT wearing a facemask. This is a positive indication that people’s choices are generally being respected and accepted by those around them in the community without incident.
A less positive finding was that only 18% of panellists believed that information about who can get an exemption to needing to wear a facemask had been made clear. A majority (68%) of panellists supported the idea of a card or other identifier that can be used by those who are exempt from wearing a facemask. This suggests that more needs to be done to communicate how facemask exemptions work and how exemptions can be signalled to the wider community. Although as noted by one panellist:
“It's important that any scheme to identify people who are exempt from wearing a mask doesn't lead to them being [negatively] targeted due to their disability or whatever reason they have for being exempt.” - AHP Panellist
Facemask Accessibility and Supply
Only 66% of panellists think they currently have easy access to facemasks while only 55% think they have affordable access to facemasks. Given the importance of widespread usage of facemasks to counter COVID-19, this suggests that more needs to be done to ensure that people are able to easily and affordably access sufficient numbers of facemasks.
figure_4.png
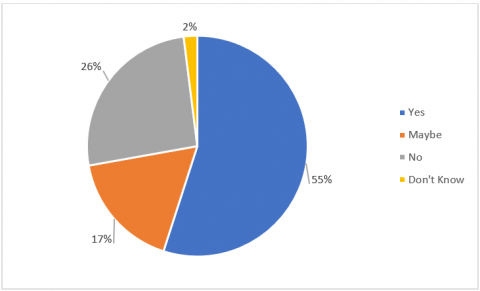
Nearly three quarters (74%) of panellists believed that the Government should mandate the supply of masks for people in high risk areas e.g. health workers, people living in ‘hotspot’ areas. Nearly 9 in 10 (87%) thought Governments should mandate the use of facemasks by those same people in the high-risk areas. Similarly, 76% said that Governments should mandate the supply of masks to all essential workers and 70% thought Governments should mandate the use of facemasks by all essential workers.
This shows that there is strong community appetite for Governments to take a much larger role in ensuring that people who are at higher risk of being infected with or transmitting COVID-19 have guaranteed access and usage of facemasks.
Changing of facemask advice
When asked about why they thought the initial Government advice that facemasks were not recommended had changed over the course of the pandemic, several common themes emerged.
The most common theme was recognition that increasing case numbers and the high rate of community transmission led to Governments changing their recommendations:
“The number of people in the community with the virus has increased and [so has] their ability to spread before they are aware.” - AHP Panellist
The recommendation about facemasks in particular was thought to change as other interventions, like social distancing and self-isolation, were not adhered to by everyone leading to increased rates and deaths. As one panellist eloquently described it:
“It [the recommendation] changed due to the large number of blasted morons deliberately ignoring restrictions, going to shops, to parties, to work when positive, people not listening, rates going up, people dying...” - AHP Panellist
The second most common theme was how the emergence of new evidence, through further research and data collection, our understanding of the COVID-19 virus which lead to changes in advice and recommendations:
“I think it [the changed recommendation] came into play after months of study giving the government more time to study how the virus really does affect others and in what ways with and without masks.” - AHP Panellist
Another common theme was the perception that the initial advice had not been based solely around health factors but took other things into account such as supply, where facemasks were initially not recommended to the public in order to assure sufficient supply to critical places and people such like healthcare workers:
“My take was that the old advice was based in an earlier time when there were supply chain shortages, so we wanted mask supplies to be preserved for use by healthcare workers."- AHP Panellist
Overall, these themes suggest that the reasons for the change in recommendations make sense to and were acceptable to the community. It is positive to see indications that the general community is aware to the changing nature of evidence and the pandemic can lead to advice changes, and that there are factors beyond health that can affect and change the best course of action going forward.
However, it was noted by panellists that the change in recommendations was not acknowledged and effectively explained, thus potentially confusing parts of the broader public with perceived inconsistency. This indicated that Government communication in this area could be improved.
“This wasn't explained well to the public - the message just changed and there was little information on why something the government repeatedly told us was unnecessary had now become necessary” - AHP Panellist
Problems, Barriers and Concerns with facemasks
When asked about what problems, barriers and concerns exist around facemask usage, panellists identified multiple common issues that need to be addressed.
In addition to the previously noted issues of cost and availability, the most common problem identified was one around accessibility. In particular the multiple groups of people who experience difficulties trying to wear facemasks including deaf/hearing impaired people, asthmatics, people with hay fever or other breathing issues, people who wear glasses and people with facial injuries such as wounds or burns.
Another commonly noted problem by panellists was one of practical usage- specifically the numbers of people they had seen wearing a mask that was a poor fit or not correctly set up to cover both mouth and nose.
A third problem identified by panellists was how physically and mentally draining extended use of facemasks could be:
“It's just exhausting and draining. I'm severely disabled and current advice is that both me AND my disability support workers should wear both face masks AND eye protection (goggles or face shield) at all times when they're working with me - that's 5 hours a day. It's physically exhausting for me because it makes it more difficult to breath and more difficult to communicate (have to speak louder, clearer, etc), but it's also psychologically exhausting - it means everybody around me looks like they're dressed up for hospital and it's quite anxiety provoking.” - AHP Panellist
The two biggest barriers identified for facemask usage were around practical instructions and cultural attitudes in Australia. Multiple panellists reported that the instructions wear to where masks, how to wear them and when to stop were not clear; making it potentially difficult for people to effectively use them to counter COVID-19. Concurrently many panellists identified fundamental aspects of Australian culture, particularly as a Western nation, as the major hurdle for adopting a population wide health measure such as facemask usage:
"Cultural - 'she'll be right mate' attitudes, freedom of speech/human rights activists who haven't been directly affected by the virus, young people who think they are invincible. The general public also view those who are wearing masks, as carriers rather than protecting themselves. Unlike some Asian countries, mask-wearing is not commonplace here in Australia and is viewed with suspicion." - AHP Panellist
Panellists expressed a wide variety of concerns about the extended usage of facemasks. The primary concerns included: health concerns that usage of facemasks would give people a false sense of safety which may result in increased risk through other behaviours, environmental concerns about the production and disposal of the large number of masks being used and safety/security concerns about large numbers of people having their face obscured and being difficult to identify or recognise.
“I am concerned with the environmental impact due to excessive use of personal protective equipment. I am also concerned mask wearing creates a false sense of security for the wearer and individuals may be less likely to engage in behavioral mechanisms to stop transmission (e.g. hand washing and social distancing).”- AHP Panellist
Open Text Feedback
In the open text response option at the end of the survey, several common items emerged from panellists’ responses.
First was criticism of about the specifics, or lack thereof, of Government communications on facemasks. This included the lack of information around exactly when and where to wear masks, how to wear masks, which masks to wear, how to care and maintain masks and how to dispose used masks. The lack of facemask usage being clearly integrated with other interventions, such as promoting hand washing and social distancing, as part of the strategy to counter COVID-19 was another perceived flaw of Government communications.
Similar criticisms were directed at a perceived lack of unity between different groups of elected representatives, in particular around Federal-State and Government-Opposition divide, with the conflicting messages around ‘mandatory’ vs ‘recommended’ vs ‘not necessary’ potentially causing much confusion amongst the Australian populace. Similarly, the perceived delay in Governments making facemasks mandatory in high risk areas such as nursing homes and health service providers was criticised by multiple panellists, with many thinking it took unacceptably long for masks to become mandatory.
Summary
Overall this survey of Australia’s Health Panel indicated that consumers largely accept that facemasks are a key part of countering the COVID-19 pandemic and know which masks are most effective. Usage of facemasks is strongly correlated with their perceived level of risk and Government requirements in the area where they live. The choices of individuals to wear or not wear a facemask are generally respected by the rest of the community but more needs to be done to clarify who is exempt from wearing facemasks. Ensuring facemasks have reliable supply and remain affordable is a key concern.
People appear accepting of changing Government requirements and recommendations as the pandemic situation develops, but desire greater clarity and consistency of messages explaining how and why things have changed. In addition, more work needs to be done to overcome practical issues affecting mask usage such as accessibility considerations and having clear instructions for how to use facemasks, as well as overcoming cultural barriers in the Australian population to such community focused public health initiatives.
“I think it is an issue of social solidarity as much as anything. It reminds us that there is a serious invisible enemy at loose and that wearing a cloth mask is not nearly as bad as having to wear full PPE as those more at risk caring for the ill must do.”- AHP Panellist
“For most people, there are few barriers [to wearing facemasks] but we need to consider providing them free of charge to low or no income earners, providing culturally acceptable information so people from CALD backgrounds understand they have to wear them, and consider people with medical reasons or disability who are unable to wear them.”- AHP Panellist
The Consumers Health Forum of Australia would like to thank all panellists for giving their time to participate in this survey. Any questions about this survey and its findings can be directed to info@chf.org.au.
Note: as each question in the AHP survey was optional, the number of responses for each question varies across the survey. As such the total ‘n’ for the set of answers of each question may not add up to the same overall number of survey participants.
