

“As a person with multiple comorbidities and on quite a few medications, pharmacy advice has been invaluable to me over the years. They [pharmacists] are a fantastic resource and should be utilised more." - AHP Panellist
I feel that we need more transparency around the pricing of prescription medicines. I have never been told the cost of a prescription before it has been dispensed, and usually discover the price when I get to the checkout. I cannot back out of the transaction, and am required to accept the price, even if it is higher than expected. I feel that this puts the pharmacist in a position of power, and has the potential to be abused. - AHP Panellist
For July 2020, following the signing of the 7th Community Pharmacy Agreement Australia’s Health Panel asked panellists about their experiences with and opinions of community pharmacy in Australia.
One hundred and sixty-five (165) panellists participated in the survey. Most were female (77%,), aged 46 or older (88%), lived in a major city (65%) and just over half (58%) identified as a person with a disability. Most panellists also self-reported as generally healthy with 27% being in ‘fair’ health, 49% in ‘good’ health and 18% in ‘excellent’ health.
Pharmacy Prices
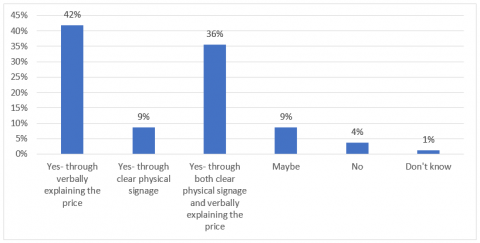
A significant majority of panellists (84%) reported that they were not told how much a prescription would cost by their pharmacist before the pharmacist dispensed it. A similar majority (84%) believed that pharmacists should be required to tell people the price of a medicine before dispensing it, although they varied on their preferred method (see Figure 1). However, most panellists believed they would be confident enough to ask the pharmacist the price if they were not told with 71% definitely being confident enough and 23% maybe being confident enough to ask.
figure_1.png
When being told a medicine price, most panellists (70%) reported they would want to be told the ‘out of pocket’ cost, although there was some interest in being given the total cost including any government subsidy (25%) or a full breakdown of the various costs and fees that make up the total cost (30%).
Just under half of panellists (49%) reported that they have “shopped around” to see if they could get their prescription medicine cheaper elsewhere, however a full quarter (25%) of panellists reported that they had never shopped around as they assumed that prescription medicines would cost the same amount at every pharmacy.
Given the above, it is promising to see that the 7CPA includes a commitment between the Pharmacy Guild and Department of Health to develop processes to ensure that pharmacists make consumers aware of prices prior to dispensing. There is clear consumer demand for greater price transparency and CHF will continue to advocate for this.
Pharmacy Services
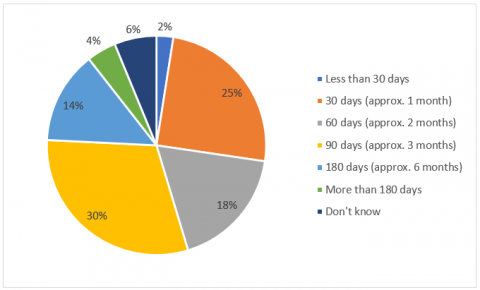
When asked what the ‘dispensing limit’ (the maximum amount of a prescription medication that can be obtained at one time) should be, only one quarter (25%) of people thought the current 30 day dispensing limit was the right maximum. The majority of panellists believed that the dispensing limit should be raised, with 18% believing it should be increased to 60 days (approx. 2 months), 30% to 90 days (approx. 3 months) and another 18% thinking it should be 180 days (approx. 6 months) or longer (see Figure 2). Given this large amount of support for increasing the dispensing limit by consumers, it is very disappointing that this was not addressed in the 7CPA and is another area CHF will continue to advocate on.
figure_2.png
A majority of panellists (73%) reported that at some point they had been unable to get a specific prescription due to a medicine shortage. However, for those affected by a medicine shortage only 69% of the time did the pharmacist explain why there was a shortage. When faced with a medicine shortage panellists responded in a mix of ways, with the most common being asking the pharmacist to order the medicine in (44%) or going to another pharmacy to see if it was in stock there (42%) (see Figure 3).
figure_3.png

Concerningly, when they last bought a prescription, 64% of panellists were not offered the Consumer Medicine Information CMI leaflet or any other information document. A clear majority (86%) thought pharmacists should be required to provide it to the consumer- either always (21%) or unless the consumer explicitly says they don’t need it (65%). This mirrors previous work done by CHF through Australia’s Health Panel over 18 months ago where 91% of panellists thought the provision of CMI leaflets should be required, indicating this is a long term and continuing issue for Australians that has not been addressed by recent changes by the Therapeutic Goods Administration (TGA) to CMIs.
While few panellists reported that they had a pharmacist do a Home Medicine Review (HMR) (only 16%), those who did largely reported positively about their experience with HMRs as being either very helpful (64%) or somewhat helpful (21%). The vast majority of HMRs were conducted in person (88%), with only three panellists reporting they’d been able to have them done via telehealth.
Similarly, only a small number of panellists (27%) had received a vaccine at a pharmacy, with the influenza vaccine being overwhelmingly the most common received vaccine at a pharmacy (94%). However, most panellists (62%) supported pharmacists being allowed to administer vaccinations.
When asked why they had obtained a vaccine through a pharmacy, the most popular reasons were due to the convenience of not needing an appointment (40%), shorter waiting time (38%) and the location being close to work/home (25%) (see Figure 4).
figure_4.png

Generally panellists thought pharmacists either currently administered the right amount of vaccines (17%), should be allowed to administer a larger variety of vaccines (27%) or simply should be able to administer all types of vaccines (19%). Very few thought they should do a smaller range (3%) or none at all (18%).
Overall this suggests that there is support from the community for pharmacists to take a more active role in delivering a broader range of healthcare services than just dispensing medicines. However, the low and narrow uptake of these broader services suggests more work is needed to increase their usage by consumers.
Pharmacy Access
When asked about programs or options to increase the accessibility of pharmacy, panellists were universal in their support for the options presented, suggesting that increasing access is a major desire for consumers currently.
In regard to the specific options discussed, a strong majority (79%) thought that the Health Care Homes program should include pharmacists and an identical majority (79%) thought Home Care Packages should include pharmacists too. Similarly, a majority (73%) thought Aged Care facilities should be able to embed pharmacists as an on-site service.
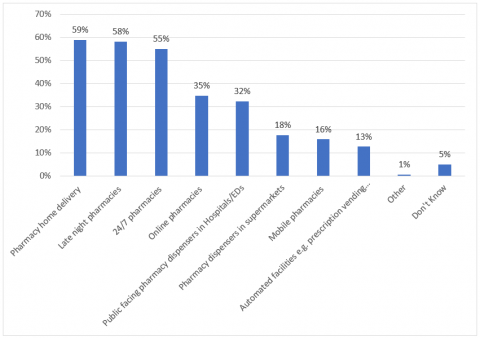
In terms of after-hours prescription facilities, an overwhelming majority (96%) wanted some form of increased option or access. The most popular specific options were pharmacy home delivery (59%), late night pharmacies (58%) and 24/7 pharmacies (55%), with online pharmacies (35%) and public facing pharmacies at hospitals/emergency departments (32%) the next most popular options (see Figure 5).
figure_5.png
Unprompted Responses
In the free text responses, several common topics emerged amongst the panellists responses:
- Local pharmacists are fantastic
Multiple panellists praised their local community pharmacist, expressing that by building a close and personal relationship with a person local to them they were able to get better service and improved health outcomes as the pharmacist knew about their conditions, gave them tailored advice and monitored their overall treatment plans.
- Generic medicines have issues
Several panellists highlighted issues with ‘generic medicines’ and did not like receiving them as an alternative for their prescription, reporting that they felt they were of a lower quality, less effective, more fragile and tasted worse than name-brand medications.
- Rural/remote regions have accessibility problems
Panellists also identified that pharmacy issues were particularly prevalent in rural and remote communities. The large distances and small populations meant that consumers have limited access to pharmacies, sometimes having no pharmacy at all in their community, reducing competition and making prices unaffordable and pharmacist services unavailable at required times.
- Pharmacies increasingly selling non-medical products is concerning
Several panellists expressed concern at the increasing number of non-medical or non-health items such as cosmetics being made available at pharmacies, likening them to becoming more akin to a ‘giftshop” than a health service setting. In a similar vein, panellists expressed concern at the provision of unproven ‘alternative medicines’ and ‘supplements’, believing this diminished the ability for pharmacists to be a trusted source of health advice and gave false support for the efficacy of such products.
- Electronic prescriptions
Multiple panellists expressed frustration that they were unable to use ePrescribing services between their GP and pharmacist to easily manage their medications. Panellists wanted increased ability to use electronic, non-paper-based records and had generally struggled to get their GPs and pharmacists to use the option effectively. Given this CHF will continue to advocate on improving ePrescribing systems as the current ‘token’ model trial comes to an end before national rollout and the ‘active script list’ model is made ready for release around October 2020.
Summary
Overall this Australia’s Health Panel indicates that consumers want more access to pharmacy e.g. pharmacy to be included in Government healthcare programs and more options by which consumers can get pharmacy products, but they also want more from pharmacy e.g. transparency of costs, longer dispensing limits and more information about medicines and shortages. While some of these consumer needs may be addressed as part of the new 7CPA agreement, many more are not explicitly targeted. CHF will continue to work with both the pharmacy sector and the Commonwealth Government to get the improvements consumers need.
My local independent pharmacy has been very helpful with my care of elderly parents - chasing up GP to make sure he has all relevant medications, explaining to me when it's best for mum to take them, asking how she's tolerating them , responding to my queries about how they might interact, etc. Very helpful and caring approach.- AHP Panellist
People should be able to access a larger volume of something like birth control pills which are taken daily, are not addictive and unlikely to be subject to overuse than say pain medication or sleeping tablets which are more likely to be abused, or may not be needed over extended periods. - AHP Panellist
The Consumers Health Forum of Australia would like to thank all panellists for giving their time to participate in this survey. Any questions about this survey and its findings can be directed to info@chf.org.au.
Note: as each question in the AHP survey was optional, the number of responses for each question varies across the survey. As such the total ‘n’ for the set of answers of each question may not add up to the same overall number of survey participants.
