“I was more relaxed in my consultation. I was in my familiar environment and the specialist and I were both at ease. I didn’t have the stress of getting the two people I care for sorted before the 90 minute drive to the city hospital for this appointment. I saved money on fuel and parking fees. I didn’t have to sit in a full waiting room. I didn’t have to turn down work for that entire day because of the travel time and waiting room time blowouts. The benefits of telehealth are immense.”- AHP panellist
During March 2020, Australia’s Health Panel (AHP) asked panellists about their views and perceptions on the use of telehealth in Australia. The survey was developed in consultation with the Consumer Health Forum’s (CHF) Rural and Remote Special Interest Group to gain an insight into the current state of telehealth in Australia. Until mid-March 2020, telehealth service in Australia were generally limited to indigenous and aged care services where patients were more than 15km from their GP. However, on the March 13 the Australian Federal Government began to expand the scope of telehealth services as part of their COVID-19 pandemic response. This culminated in an announcement on the March 29 that telehealth would become an option available to all Australians. Consequently, the AHP survey was extended into April 2020 to allow for more people to have their say on telehealth as it entered prominence in the broader public discourse.
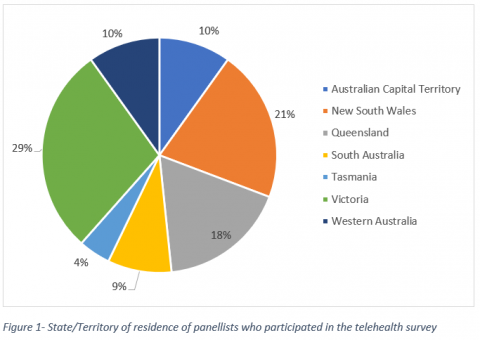
Overall, 95 panellists participated in this survey, with most of them being female (74%, n=68) and aged 46 or older (90%, n=82). Interestingly 44% (n=40) were aged 65 or older, putting them in a demographic more likely to have engaged in telehealth before the COVID-19 pandemic. Most participating panellists lived in major cities with more than 250,000 people (65%, n=59) with a broad spread across every State and Territory except for the NT (see Figure 1).
Of those who participated in the survey, the vast majority (98%, n=91) had heard of telehealth but only one third (34%, n=32) had ever been offered a telehealth service as an option for their healthcare. However, of those who have been offered a telehealth service, a significant majority of 88% (n=26) had ended up using that service. This suggests that people are generally very aware of telehealth as a concept and very willing to use telehealth services but are not generally being offered them as an option by healthcare providers.
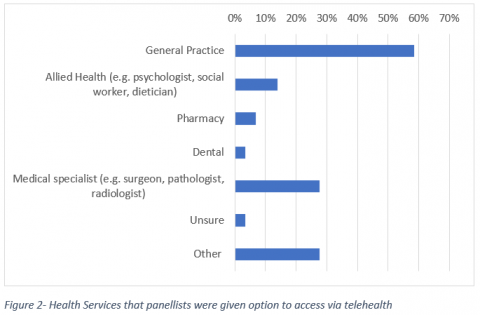
The two most common types of healthcare service consumers were offered via telehealth were for general practice (59%, n=17) and medical specialists (28%, n=8). Other common health services such as allied health, pharmacies and dentists had very limited offerings of telehealth (see Figure 2). In addition, some individual panellists reported the use of telehealth to access other services such as endocrinology, palliative care, homeopathy and “emergency information”.
The majority of panellists that used telehealth services found it to be of excellent or good quality (82%, n=23), with only one person reporting it be ‘poor’ and none reporting it as ‘very poor’. When compared to regular face-to-face consultations however the panellists were more split: 39% (n=11) believed it was better than face-to-face, 32% (n=9) thought it was worse and 29% (n=8) thought it was more or less the same. Common problems for telehealth included health professionals not embracing the option effectively, technological problems with phone or internet lines, and concern about missing services that could only be done face-to-face, for example, physical examination.
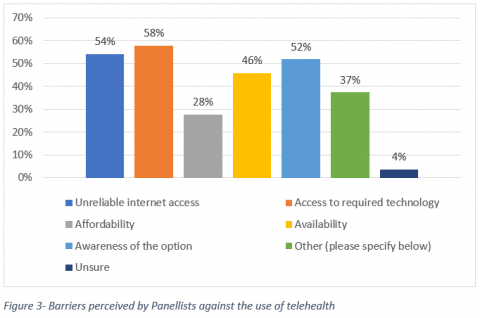
These issues that panellists had experienced with their own uses of telehealth lined up with the broader perception amongst panellists of the current barriers of telehealth. The three largest perceived barriers were ‘access to required technology’ (58%, n=48), ‘unreliable internet access’ (54%, n=45) and ‘awareness of the option’ (52%, n=43). The full list of options can be seen in Figure 3, with the ‘other’ barriers including health practitioners not embracing telehealth, MBS items still being too restrictive, privacy concerns, a lack of appropriate facilities at health providers to enable delivery of telehealth services, and a fear of reduced quality of service as healthcare providers use telehealth to cut costs.
However even with these perceived barriers, the majority of panellists reported that they were likely or would definitely use telehealth services in the future (83%, n=74), with only a single panellist reporting that they definitely would not use telehealth services. Panellists reported multiple reasons in favour of using telehealth. These included: convenience e.g. easier appointment times and no need to travel to the doctor, improved accessibility e.g. access to new types of health services and access from remote/regional locations, and personal health safety e.g. not having to spend time in the waiting room with other sick people.
In summary, this survey on Australia’s Health Panel suggests that Australians are aware of telehealth as an option for their healthcare and are generally eager to embrace it for the own health services. However, they have concerns about whether there are appropriate technological infrastructure and healthcare professional skills to ensure that telehealth services are able to be delivered appropriately and effectively.
As we move into a post-COVID-19 world, based on this Australia’s Health Panel survey we would recommend that the Australian Government looks to continue to support whole-of-population telehealth and looks to further develop the infrastructure and training to ensure it is an effective part of a 21st century healthcare system.
The Consumers Health Forum of Australia would like to thank all panellists for giving their time to participate in this survey. Any questions about this survey and its findings can be directed to info@chf.org.au.
“Each and every health facility should have a video link set up to connect the patient and health care professional, with software developed and approved by the Australian Govt. The Australian Govt must set this up as a matter of priority to allow for quality links between patients and health professionals. This however must never be in place of a real face to face visit with the patient if this is what the patient wants”- A member of Australia’s Health Panel.
Note- as each question in the AHP survey was optional, the number of responses for each question varies across the survey. As such the total ‘n’ for the set of answers of a question may not add up to the same overall number as other questions.