

"I believe I am a very well informed consumer but I sometimes struggle to understand what is being said. I can only imagine how difficult it is for those people who have less knowledge or come from a non-English speaking background. Clinicians come from a position of power - they need to acknowledge this and reach out to consumers to partner in their care. This is assisted by a strong consumer voice." -AHP Panellist
“Medical terminology can be confusing. When a person I know received his diagnosis of atrial fibrillation he thought he had a severe cardiac condition. It wasn't until he consulted a Cardiologist that he was informed it was not dire and he could continue with moderate exercise, healthy diet and minimal medication.” -AHP Panellist
For October and November 2020 Australia’s Health Panel (AHP) looked at the use of jargon in the Australian healthcare system, building on the ‘Drop the Jargon’ campaign as part of Health Literacy Month. Drop the Jargon is an initiative that brings attention to the language used by workers in the health and human services sector that is often not understood by consumers. The campaign encourages professionals in Australian health, community services and government to use ‘plain language’ to ensure people understand what it being said.
This AHP survey consisted of two parts. The first part of the survey was a short multiple-choice-quiz asking panellists to identify the correct definition for 15 pieces of medical jargon or indicate that they did not know what the term meant. The 15 terms used in the quiz were selected in consultation with the CHF Research and Data Special Interest Group.
The second part of the survey had panellists recount their own experiences with the use of jargon and their views on what barriers exist for ensuring consumers understand their health status and their healthcare.
Demographics
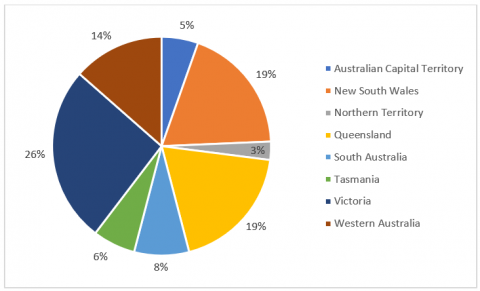
This Australia’s Health Panel survey had 121 panellists participate. They were mostly female (80%), skewed older with 46% aged 46-65 and 42% aged over 65. Two thirds (66%) of the participating panellists lived in major cities (more than 250,000 people) and they hailed from all States and Territories of Australia (see Figure 1).
figure_1.png
Participating panellists self-reported as being in good health status, with 64% being in either excellent or good health. Nearly half (48%) identified as a Person with a Disability (PwD) and nearly a quarter (22%) were Culturally and Linguistically Diverse (CALD). 7% identified as LGBTIQA+ and 2% as Aboriginal or Torres Strait Islander (ATSI).
Drop the Jargon Quiz
As can be seen in Table 1, panellists were largely successful in correctly identifying the correct meaning of the jargon terms in our Drop the Jargon Quiz- with 80% of more correctly answering for nine of the 15 terms.
| Jargon | Definition/Meaning | Correct | Incorrect | "Don't Know" |
|---|---|---|---|---|
| Sutures | Stitches | 100% | 0% | 0% |
| Hypertension | High blood pressure | 99% | 1% | 0% |
| Ambulatory | Able to walk around | 93% | 4% | 3% |
| "Negative" test results | The results show that the condition being tested for is not present | 93% | 5% | 2% |
| Haemorrhage | Blood loss from a broken blood vessel | 92% | 7% | 1% |
| Echocardiogram | An ultrasound of the heart | 88% | 4% | 9% |
| Acute condition | A condition that is sudden and short | 86% | 12% | 2% |
| Edema | Swelling | 85% | 9% | 6% |
| Atypical condition | A condition that is not normal | 80% | 17% | 4% |
| Idiopathic illness | An illness with an unknown cause | 71% | 11% | 18% |
| "PT" | Physiotherapy | 59% | 13% | 28% |
| Tachycardia | Rapid heart rate | 55% | 34% | 11% |
| Compound fracture | A bone that has broken and sticks out of the skin | 45% | 46% | 9% |
| Take a medicine "a.c." | You must take it before meals | 35% | 7% | 58% |
| Comminuted fracture | A bone that has broken into many pieces | 33% | 23% | 44% |
However, for the remaining six terms significant proportions of panellists either answered with an incorrect option and/or did not know what the term meant. And for half of those (or one fifth of the overall 15 piece of jargon), only a minority of panellists selected the correct response. In addition, when asked how confident they were with their responses just over half of panellists (53%) said that they were only ‘Somewhat confident’ while only 10% were ‘Extremely confident’ (see Figure 2).
figure_2.png
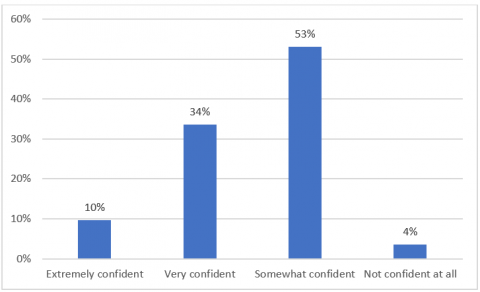
Overall this suggests that while panellists were generally successful at correctly identifying what medical jargon terminology meant; there were still terms that they did not know. And even if they did understand the meaning, they may have some uncertainty as to whether they were correct. This strongly suggests the potential for miscommunications to arise in healthcare settings and less-than-optimal health outcomes.
Panellists were almost unanimous in believing health literacy is important for getting safe, effective and quality healthcare with 97% saying it was either ‘Extremely important’ or ‘Very important’. Similarly an overwhelming majority of panellists believed that health literacy is either ‘Extremely important’ (59%) or ‘Very important’ (33%).
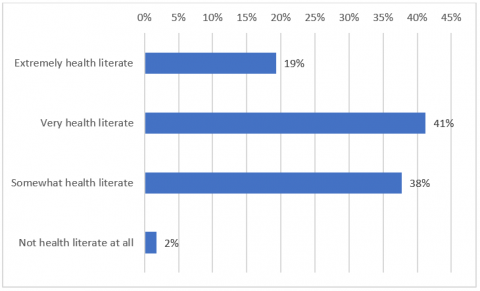
This is makes the Jargon Quiz results particularly pertinent when considering that the panellists largely self-reported as being health literate, with 19% self-reporting as ‘Extremely health literate’ and 41% reporting as ‘Very health literate’ (see Figure 3). This suggests that in segments of the Australian population with lower levels of health literacy, the ability to confidently understand the terminology being used would be lower and the risks of uncertainty and miscommunication would be more pronounced.
figure_3.png
Healthcare Experiences
When asked if they had ever struggled to understand what a health professional was saying due to the word or terminology they used; a significant majority of 73% of panellists responded that they had. While not directly comparable, this did mirror the results of the ABS 2018 Health Literacy Survey where people reported it was usually easy (56%) or always easy (33%) to actively engage with healthcare providers and they found it usually easy (54%) or always easy (39%) to understand health information well enough to know what to do. Indicating that while things were potentially fine most of the time, the majority of people have some negative experience at some point.
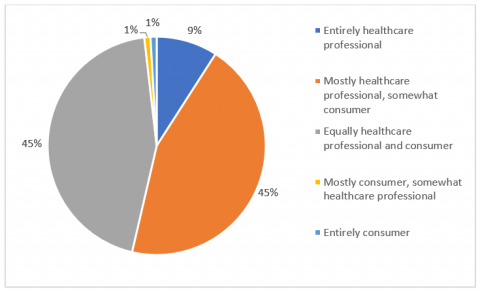
The panellists were split as to how responsibility should be divided for making sure a consumer understands what is happening with their health and healthcare. 45% believed that it was equal part responsibility between the consumer and the healthcare professional, while another 45% believed it was mostly the responsibility of the healthcare profession and only somewhat the responsibility of the consumer. A further 9% responded that it was entirely the responsibility of the healthcare professional. Overall this suggests that while most consumers do take on some level of responsibility of making sure they fully understand what is happening with their health, there is an expectation that healthcare professionals will take the lead in making sure communication is clear and full understanding is achieved (see Figure 4).
figure_4.png
Interestingly, when asked what they would do when they didn’t understand what a health professional meant or were struggling to understand some health terminology, the three most common options were; ‘check with the healthcare professional straight away’ (78%), ‘check online’ (51%) and ‘check with another health professional’ (20%) (see Figure 5). However when asked what they would do FIRST, 82% reported they would ask the health professional straight away. This was almost an order of magnitude larger than the second option of check online (11%), which itself was another order of magnitude greater that the third option ‘ask another health professional’ (2%).
figure_5.png
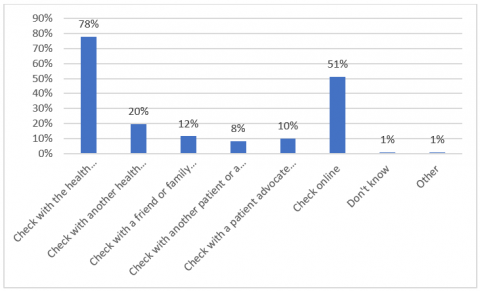
This indicates that health professionals themselves are the best placed to be the conduit by which consumers can resolve their misunderstandings about their health status, but that ensuring accurate and understandable information is easily findable online is an important back-up option.
Barriers
When asked what barriers they believe existed for ensuring health professionals and consumers understood each other, several themes emerged. Perhaps unsurprisingly, one of the more common themes were a lack of time in health appointments, with dozens of panellists identifying time constraints as a major barrier. As one panellist described simply:
Health professionals are often very busy and rushed during appointments which does not often allow time to explain the details.
Equally common was the barrier of language and culture, with the varying level of English skill amongst both consumers and healthcare practitioners, as well as accents for both, cited by many.
Being from a non-English background also impacts on ability to question and indeed understand. Culture is also important - if we are used to being told that clinicians are the professionals we are less willing to be active participants.
Concerningly many panellists also noted unhelpful attitudes of health practitioners not wanting to be questioned by consumers as a barrier, especially when compounded with consumers feeling nervous or uncomfortable to speak up.
I think there are preconceptions about the other's role - it is often an uneven relationship - some health professionals feel superior or are arrogant, don't like to be questioned, or are too busy to take the time to explain their decisions. Patients are sometimes too timid, feel it is not their place to question or challenge or are in too much pain, worry or fearful to think straight and often don't know what questions to ask.
Many consumers feel intimidated by health care professionals and feel awkward or feel time pressure and do not seek clarification.
Mental health was a specific area where panellists highlighted barriers, with consumers historically being disempowered and disregarded, leading to poor understanding:
Dis-empowered mental health consumers are often made to feel that they're [sic] opinion doesn't matter so often their understanding isn't considered either.
Some more basic barriers identified were the amount of assumed knowledge health professionals often expected consumers to have and a reliance on written materials to explain concepts to consumers:
Health professionals may say the same things repeatedly, speak fast, in language they themselves understand but not appreciating this is the first time for the patient receiving the information.
Clinicians rely on written materials, assuming (WRONGLY) that consumers will/can read and understand and then ask questions. Also, clinicians are time-poor, so do the least feasible work on comprehension and understanding, and rarely check in with consumers.
The condition of the consumers at the moment of the consultation and generally low health literacy were also recurring barriers noted by panellists, with the former impacting the ability of consumers to understand information in the moment while the later was a backdrop upon which consumer misunderstandings could easily arise:
If the patient is tired, groggy from medicine or anaesthetics or in shock because we can't retain information, no matter how simple, under these circumstances.
Many consumers are not health literate and not all health professionals know how to make the conversation understandable.
Overcoming Barriers
In order to overcome those barriers, the panellists suggested a range of items that boiled down to three recurring categories.
The first of these was further training and education for health practitioners, the give them the awareness of topics such as cultural considerations and equip them with skills to more effectively engage with consumers. Multiple panellists made explicit reference to not only needing to reframe the language and word choices used but the need to switch the discourse to one of two-way questioning. Where doctors don’t ask ‘if they understand’ but instead ask the consumer to explain back to the doctor what is happening and ask questions of the doctor. Resources like the ‘Five questions to ask your doctor’ were highlighted as valuable tools that should be used more often to prompt consumers into feeling comfortable to ask questions of their health providers.
The second recurring category was that of improving the health literacy of the broader public. Suggestions for doing so ranged from content in high school curriculum to community courses to the provision of a broader array of better designed resources in health clinics.
The final category was one of broader systemic change and improved resourcing- this included increasing the Medicare rebate and allowing for longer appointment times, providing translators and other support for consumers to draw upon (such as encouraging them to bring a friend or family member to an appointment) and ensuring information is provided in multiple formats to best meet consumer preferences.
Although several panellists noted that doctors and health professionals don’t all individually need to be great communicators, that the overall system should have avenues available to balance out those whose strengths lie in other parts of healthcare:
Occasionally one finds a health professional who is extremely competent but not very good at communicating (often a surgeon). In this case, it makes more sense to ask questions of one's own GP or a nurse, as surgeons' expertise lies in the theatre rather than in communication. I do not believe it is essential that all health professionals be brilliant communicators, as long as there is someone around who can fill the gap
Conclusion
In summary, although it is likely the respondents to the survey were towards the higher end of the health literacy spectrum, the panellists who participated had gaps in their responses to the Jargon Quiz, and a significant majority reported that they had at some point struggled to understand what a doctor was saying to them. Most panellists believed that both consumers and health professionals had shared responsibility to ensure understanding, although they were split between equal responsibility or believing responsibility mostly rested with health professionals. Given this, and that panellists overwhelmingly reported that they would immediately ask the health professional if they were uncertain about some details, health professionals are ideally placed to take the lead in ensuring consumers fully understand the specifics of their health status and healthcare. This should involve the use of tools and practices such as shared decision-making to activate and empower patients. Ensuring accurate and understandable information is easily sourced online is a recommended back-up for when consumers do not seek clarity from the health professional directly. Given the proliferation of health information online, it is important that consumers are given guidance so they are able to discern the better, more evidence-based health information on line.
The range of barriers identified by panellists align with what has been previously identified and add support to many of CHF’s current projects. For example our current NPS-CHF Partnership project contains activities to improve health literacy, our advocacy in the negotiations for the Seventh Community Pharmacy Agreement on the need to improve the provision of information to consumers, our #BeHealthAware health literacy portal and the ongoing work of our Safety and Quality Special Interest Group who work with a range of organisations to improve the larger system of consumer communications. The results of this survey will feed directly into those and other CHF work to inform our advocacy effects.
Abbreviations, Acronyms and Jargon have no place in important patient discussions. Coupled with either a clinician or patients' unquestioning attitude, can leave patients disempowered. Use of medical terminology can also be used as a shield to avoid meaningful but difficult discussions. Sometimes, they are also used to blame patients for not understanding. Years of conditioning has made a huge portion of patients dependant on clinicians to make them well. Yet, we know that engaged patients and families have safer and better health outcomes. Most patients don't know this. Clinicians can help patients by improving their communication and by encouraging patients to have active roles in their own health and healing.
The Consumers Health Forum of Australia would like to thank all panellists for giving their time to participate in this survey. Any questions about this survey and its findings can be directed to info@chf.org.au
Note: as each question in the AHP survey was optional, the number of responses for each question varies across the survey. As such the total ‘n’ for the set of answers of each question may not add up to the same overall number of survey participants.
